Sommaire
What solutions exist for measuring CO2?

There is growing evidence that high levels of carbon dioxide increase the risk of airborne infection. Carbon dioxide is produced by the exhaled air of people in enclosed spaces. Each person in a building breathes about eight liters of air per minute: air that was in close contact with lung tissue. In addition to CO2, at a concentration of around 40,000 ppm (“parts per million”), exhaust air also contains tiny liquid droplets (aerosols) which, because of their size, can float in the air. These droplets also contain the viral particles present in the lungs. CO2 sensors can reduce the risk of infection.
Il est supposé que la vitesse de descente des aérosols est généralement de quelques mètres par heure. La diminution des virus biologiques a une demi-vie d’environ trois heures dans des conditions de laboratoire. C’est-à-dire que l’air ambiant reste pollué pendant une longue période.If a healthy person breathes in these contaminated droplets, and the number of viral particles they contain exceeds a minimal dose of infection, disease is transmitted. As direct measurement of the viral load is difficult, maintenance-free sensors are an ideal way of monitoring CO2 concentration and thus preventing the build-up of consumed air.
CO2 content as an indicator of covid-19 transmission risk

Airborne transmission appears to be a major factor in the spread of the virus. Consequently, CO2 levels in premises can be used as an indicator of the risk of COVID-19 transmission.
“Since the Corona virus is airborne, higher CO2 levels in a room likely mean a higher risk of transmission if an infected person is indoors,” writes leading aerosol scientist Professor Shelly Miller in The Conversation.” Simply put, the more fresh air brought in, the better the air quality. Introducing that air reduces the infectious load, whether it’s a virus or other things, and reduces the exposure of the people in the building.”
A 2019 study of a tuberculosis outbreak at Taipei University (Taiwan) provides detailed evidence. Many rooms were poorly ventilated and reached CO2 levels in excess of 3,000 ppm. When engineers reduced the values to below 600 ppm, the epidemic was halted.
What is the right CO2 content for a safe environment?
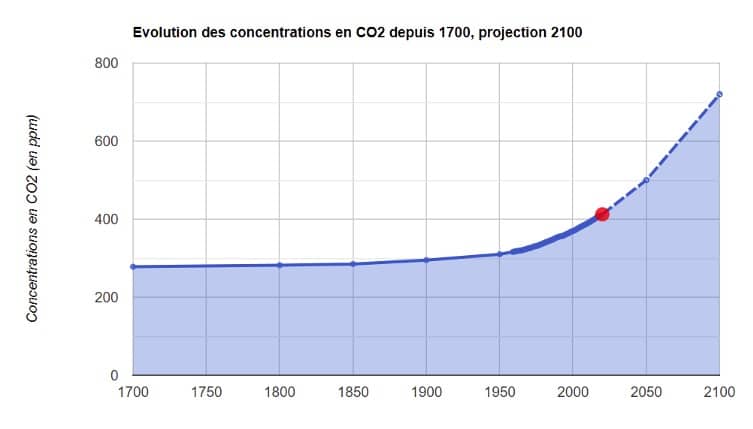
For comparison, in the 21st century, outdoor air contains around 0.04% CO2, or 415 ppm (parts per million). Scientists propose a guideline value of 1000 ppm for the use of CO2 as a VOCID-19 indicator in classrooms. They argue that transmission at space level is the key. The amount of virus in the air can increase, leading to increased exposure. If you stay in a poorly ventilated room for a long time, you run a fairly high risk, even if you stay at a distance, because the air moves.
Indoor CO2 measurements are easy to install with affordable sensors, for large-scale monitoring of the risk of indoor aerosol transmission for Covid-19 and other respiratory diseases. Nevertheless, it seems useful to set differentiated C02 reference values for each case.
Indeed, depending on the environment and the type of activity, the risk of infection has been shown to vary greatly. Factors such as the number of infected people in a given area and measures such as wearing masks or air purification can reduce the viral load in ambient air without reducing the constant CO2. What’s more, activities such as talking, singing and shouting increase viral emissions far more than CO2 concentration. Ventilation and fresh air reduce both CO2 and viral load. This is not the case with air recirculation or air purification, for example, which reduce the viral load but have no impact on CO2 levels.
CO2 content and containment index
If we’re in a room with several people, measuring CO2 content provides a good indication of the percentage of the air we inhale that has already been inhaled by other people. For example, a measured CO2 concentration of around 1200 ppm means that almost 2% of the ambient air has already come into contact with the lungs. So, one in every 50 breaths is made up of air already exhaled. However, it is not possible to directly deduce a specific risk of infection with COVID-19. It depends on various factors that are still the subject of intense research. Nevertheless, CO2 measurement is a pragmatic and cost-effective solution for estimating the current risk of potentially infectious aerosols.
Strategies to reduce the risk of infection[DB2].

A CO2 concentration of <1000 ppm is hygienic. Concentrations between 1000 and 2000 ppm are considered to be of concern. Above this level, the concentration is unacceptable. CO2 is also an important reference for infection prevention in nursery schools.
In Germany, for example, the “Ventilation” working group of the UBA (Federal Office for the Environment) recommends the use of traffic lights indicating C02 concentration. The DGVU goes even further, advocating a target value of 700 ppm in classrooms during the pandemic phase.
Aérer ne signifie pas seulement un échange d’air, mais aussi une perte de chaleur en hiver. Une stratégie durable devrait également tenir compte de cet effet. Là où il n’y a pas de climatisation moderne avec échangeur de chaleur, seule la surveillance du CO2 et une ventilation manuelle orientée sur la demande ou régulière aident.REHVA, the Association of European Heating, Ventilation and Air Conditioning Associations, is calling for the installation of CO2 monitors with warning lights in classrooms, “particularly in schools where window ventilation depends on windows and/or grilles”.
Also read: Our air purifiers are effective against Covid-19 in nurseries, kindergartens, schools and colleges.
Installation of CO2 sensors
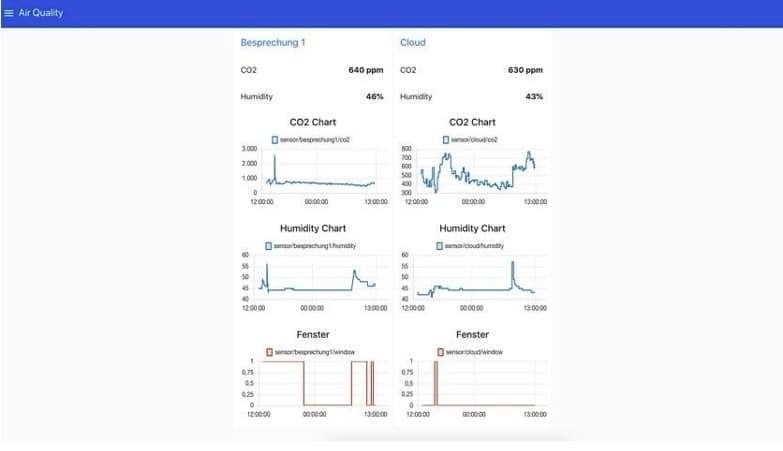
To meet these requirements, reliable CO2 sensors must produce results and be easy to install where they are needed. Ideally, they are connected, for example to prevent alarm when CO2 concentration exceeds “traffic light” thresholds, and send this message to building management networks or wirelessly to smartphones. Maintenance-free sensors are ideal for these purposes. These solutions enable continuous monitoring of CO2 concentration in ambient air, without the need for special installation or wiring.
Sources
Is there a link between CO2 and the transmission of the COVID-19 virus (what do scientific studies have to say about this)?
Each person exhales around 8 to 10 liters of air per minute, which has been in intensive contact with lung tissue. In addition to CO2 (4% = 40,000 ppm), exhaled air therefore also contains tiny droplets (aerosols) which, because of their size, can float in the air for a long time. If the person in question is infected with the virus, these droplets will also contain viral particles. Aerosols descend at a speed of a few meters per hour, and the reduction in biological viral infection activity is around 2.7 hours, so the ambient air remains polluted for longer. If a healthy person inhales these contaminated droplets, and the number of viral particles they contain exceeds a minimal infectious dose, the disease is transmitted. Over 200 scientists recently called on the WHO to take the airborne transmission of SARS-CoV-2 more seriously (Morawska & Milton, 2020)…
Where is the best place to position your CO2 sensor?
To get the most out of your CO2 sensor, it’s important to place it at face height, ideally between 1 and 2 meters. However, don’t place the CO2 sensor near a person (next to a desk, for example), as this may distort the results, as the person breathing will automatically generate CO2 near the sensor. You should also be careful not to place the CO2 sensor near a window, door or air vent.
